If you have healthy eyes, it can be easy to forget about common eye diseases, such as glaucoma. Why should you be concerned about them when they don’t affect you? There are some eye conditions, such as glaucoma, that can cause vision loss that you don’t even notice until it is too late.
While eye diseases develop differently, glaucoma is a common condition that can be hereditary. If someone in your immediate family has glaucoma, it’s something you should test for as soon as your optometrist recommends.
Although genetics plays a part in developing glaucoma, not everyone with a family history of the disease will get it. There are other risk factors to consider.
Even if a grandparent, parent, aunt, or uncle develops glaucoma, it’s not guaranteed that you’ll get it, too. However, family history is relevant in your eye exams.
What Is Glaucoma?
Glaucoma is a group of eye diseases that damage the optic nerve, the part of the eye that communicates what you see to the brain. There’s no clear cause of glaucoma, but it’s linked to an imbalance of eye pressure, referred to as intraocular pressure (IOP). The imbalance is caused by too much fluid entering the eye, not enough fluid exiting the eye, or an imbalance of pressures around the optic nerve.
Pressure imbalance causes damage to the optic nerve at the back of the eye over time. Once the optic nerve is damaged, it can’t effectively communicate what your eyes are seeing to your brain, leading to partial or complete vision loss.
There are several variations of glaucoma, some more common than others.
Open-Angle Glaucoma
Open-angle glaucoma is the most common type and accounts for 90% of glaucoma cases. A lot of the time, people don’t realize they have this type of glaucoma because it develops very slowly. Detecting this type of glaucoma early with regular eye exams is essential because it can cause vision loss that is irreversible like all types of glaucoma.
Acute Angle-Closure Glaucoma
Also referred to as acute glaucoma, angle closure glaucoma has sudden fluid blockage from the iris (colored part of the eye) that can’t drain out of the front of the eye. IOP spikes quickly, causing eye pain, red eyes, and blurry vision. Acute angle-closure glaucoma is a true eye emergency and can lead to blindness if not treated right away.
Chronic Angle-Closure Glaucoma
Much like acute angle closure, chronic angle-closure glaucoma occurs when the iris blocks the eye’s drainage angle. This causes pressure inside the eye to increase intermittently and can lead to optic nerve damage. This can occur with or without eye pain and usually, vision loss occurs slowly over time so it can also go unnoticed.
Normal-Tension Glaucoma
Normal tension glaucoma can develop even when IOP is normal. It may occur due to low blood pressure but is caused by an imbalance of fluids surrounding the optic nerve and the exact mechanism is unknown. It is more difficult to detect and is usually found by careful optic nerve evaluation by an eye care professional.
What Are the Symptoms of Glaucoma?
Those with glaucoma have little to no symptoms. Plenty of people live their lives without even knowing they have it. The symptoms start slowly and gradually grow more intense. This is one of the reasons why routine eye exams are so important.
Your optometrist can detect glaucoma if you’re experiencing symptoms such as:
- Gradual loss of peripheral vision
- Tunnel vision
- Eye pain
- Blurred vision
- Halos around lights
Most of the time people with glaucoma have no symptoms at all. It is very important to have your eyes evaluated regularly, especially if you have a family history with glaucoma.
Is Glaucoma Hereditary?
Although anyone can develop glaucoma, your family history plays a key role in your risk of developing it. Early onset glaucoma appears before age 40 and has a strong heritable component. Primary open-angle glaucoma is commonly passed down through families. If you have a family history of glaucoma, your optometrist will start screening for the disease earlier than usual.
Structural differences in the eyes are also inherited, which can make you more susceptible to developing glaucoma. IOP is often affected by physical abnormalities that block fluid drainage in the eyes.
Babies can also be born with eye problems that affect normal fluid drainage, leading to congenital glaucoma, which is seen in roughly every 1 in 10,000 babies. While rare, the signs generally become apparent right away.
Babies born with congenital glaucoma:
- Make extra tears
- Have clouded eyes
- Are sensitive to light
Other Risk Factors for Glaucoma
Genetics isn’t the only factor at play in the development of glaucoma. Other risk factors include:
- Age (over 40)
- Diabetes, high blood pressure, or low blood circulation
- High myopia (nearsightedness)
- Previous eye injuries
- Thin corneas
Whether you have a family history or other risk factors, optometrists can easily check for glaucoma during a comprehensive eye exam.
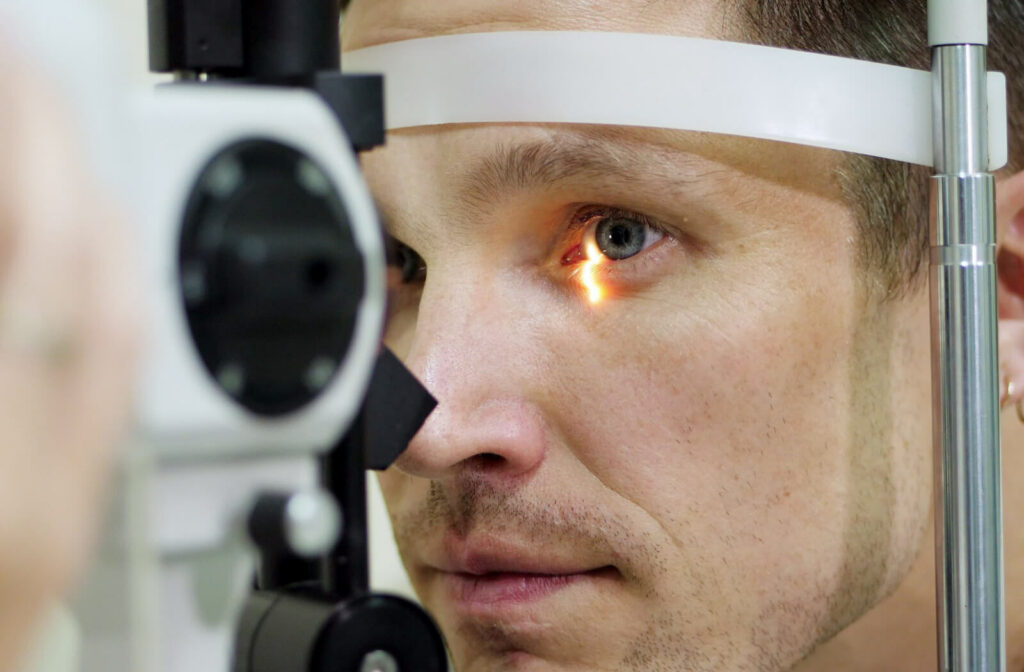
How Does an Optometrist Diagnose Glaucoma?
Optometrists use several tests to look for signs of glaucoma.
Tonometry
The gold standard of glaucoma tests, Goldmann applanation tonometry is a diagnostic tool that measures IOP by gently pressing a probe against the eye’s surface.
Other types of tonometry use non-contact methods, such as a puff of air, to determine the cornea’s response. If the test results are abnormal, optometrists have other tests to confirm a diagnosis:
- Optical Coherence Tomography (OCT): measures the thickness of the nerve fiber layer of the optic nerve
- Ophthalmoscopy: carefully evaluates the optic nerve after dilation
- Perimetry: tests the whole field of vision for areas of vision loss
- Pachymetry: inspects the thickness of the cornea
- Gonioscopy: examines the drainage angle of the eye
Who Needs a Test for Glaucoma?
Just having a family member with glaucoma doesn’t mean you’re guaranteed to develop the disease, too. However, if you have a family history, you should maintain a regular eye exam schedule and tell your optometrist your family history.
Treatment options are available, from prescription eye drops to surgery. Following a comprehensive eye examination, our specialized optometrists can advise you on the best course of treatment.
If you’re concerned about glaucoma, contact Heartland Eye Consultants to learn more about how we can help you.